MIT researchers have developed injectable “mini livers” that function as satellite organs, potentially transforming treatment for liver failure. Built using hydrogel microspheres, the technology showed sustained function in animal studies and may reduce dependence on donor organ transplants.
Published Date – 26 April 2026, 12:38 PM
Hyderabad: In a breakthrough that has the potential to redefine the treatment of end-stage liver failure, engineers at the Massachusetts Institute of Technology (MIT) have developed injectable ‘mini livers’.
The engineered tissues, described as ‘satellite livers’, are designed to be deployed (injected) into the body to supplement the functions of a failing organ like liver without the need for invasive transplant surgery.
Published in the journal Cell Biomaterials, the study offers hope to thousands of patients, including those in India, who are caught in the waiting list for donor organs and have to wait for multiple years or are too weak to survive a major transplant surgery.
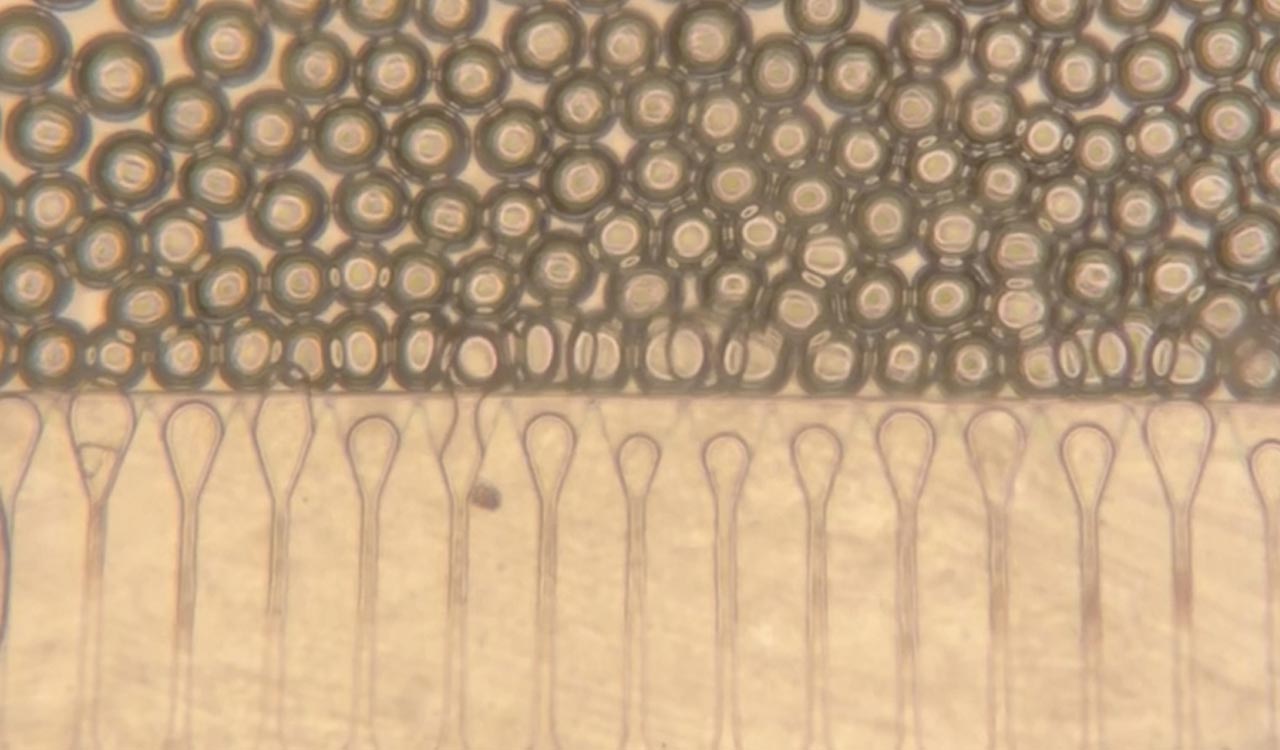
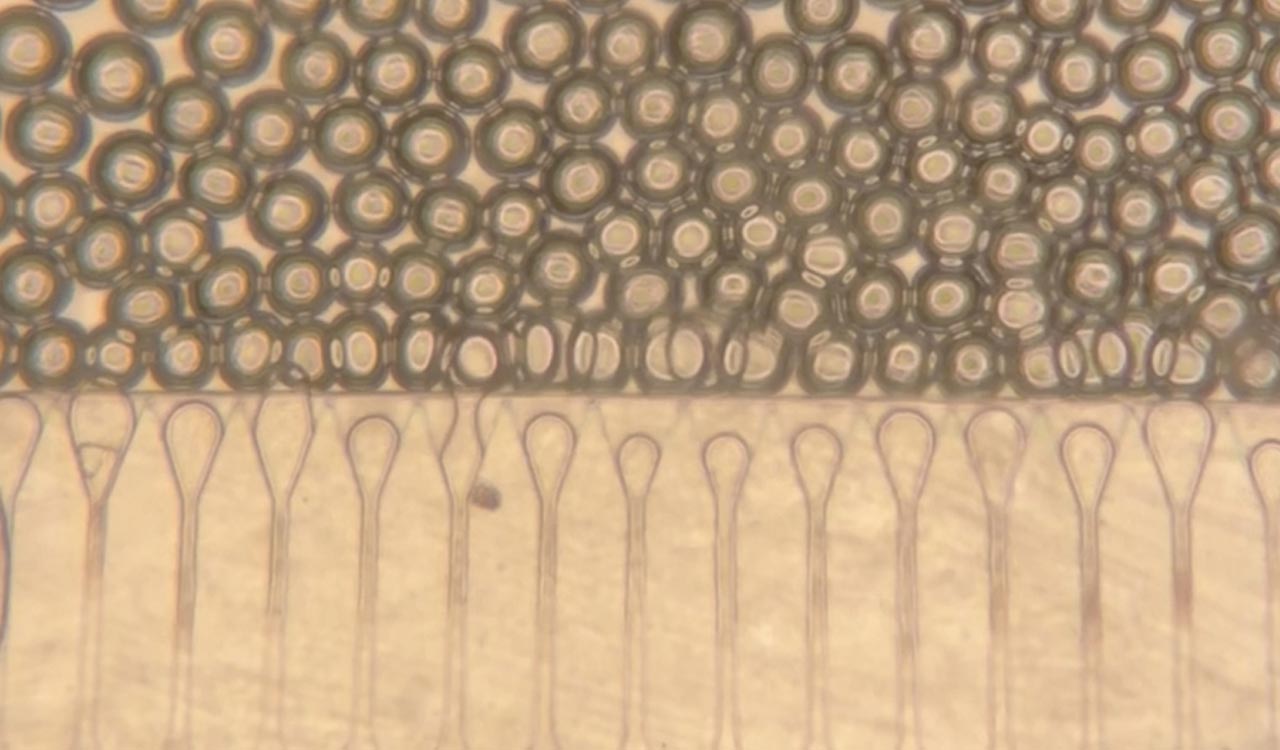
The primary challenge in liver cell transplantation has always been survival; once injected, cells typically struggle to find blood supply and die. The MIT team, led by Professor Sangeeta Bhatia and postdoc Vardhman Kumar, solved this by embedding human hepatocytes (liver cells) into specialized hydrogel microspheres.
These microspheres behave like a liquid when pushed through a syringe but instantly reorganize into a solid, supportive scaffold once inside the body. The microspheres encourage the body to grow new blood vessels directly into the graft, connecting the mini-organ to the host’s circulation within days.
In animal models, these satellite livers remained functional for over two months, successfully producing essential proteins and enzymes. Crucially, the researchers found that these grafts do not need to be placed near the original liver; they functioned perfectly when injected into fat tissue in the abdomen.
While the current version requires immunosuppressants, the team is working on stealth cells to evade immune detection. For similar patients in Telangana and elsewhere in the country, where organ demand far outstrips supply, the ‘mini liver’ technology could serve as a vital ‘bridge’, keeping patients stable until a donor organ becomes available.